We Were Lucky Enough to Have Prenatal Care that Saved Our Lives. It Shouldn’t Be About Luck.
Six weeks into my first pregnancy, I found out I had an enlarged placenta. My doctor assured me it was likely nothing but told us it was important to keep an eye on it.
Although I didn’t know it then, “keeping an eye on it” probably saved my son’s life. And mine.
That’s because, from the very beginning, we had the medical and financial support to not just stay healthy, but to survive. For too many women around the world, that’s far from a given.
Like every expectant parent, I was nervous. But I was also optimistic—even though “keeping an eye on it” meant that when my pregnancy reached 32 weeks, I’d need fetal non-stress tests three times a week, in addition to my regular prenatal appointments, to check the baby’s heart rate. Still, the monitoring seemed like a formality.
One warm September afternoon, as I relaxed into a giant easy chair at the maternal-fetal medicine clinic, I felt good. There was zero indication of anything wrong.
The nurse positioned electrodes on my belly and a blood pressure cuff on my arm.
My blood pressure started high and rose quickly. The nurse checked my charts and monitored my readings. By the time my blood pressure hit 160/90, I started to panic.
I was experiencing preeclampsia—a fancy word for high blood pressure that occurs after the 20th week of pregnancy or soon after delivery. It’s rare but serious. Untreated, preeclampsia can cause serious, even fatal complications such as seizures for both mother and baby. While preeclampsia can be managed, the only treatment is delivery.
I was immediately admitted to the hospital. Doctors told me that if my blood pressure continued to go up, my 32-week-old baby was going to be delivered.
In my hospital room, things got worse, fast. My blood pressure kept climbing. My liver enzymes rose, and my blood platelets dropped—signs of a dangerous variant of preeclampsia. My baby could die. I could die.
They prepared me for delivery.
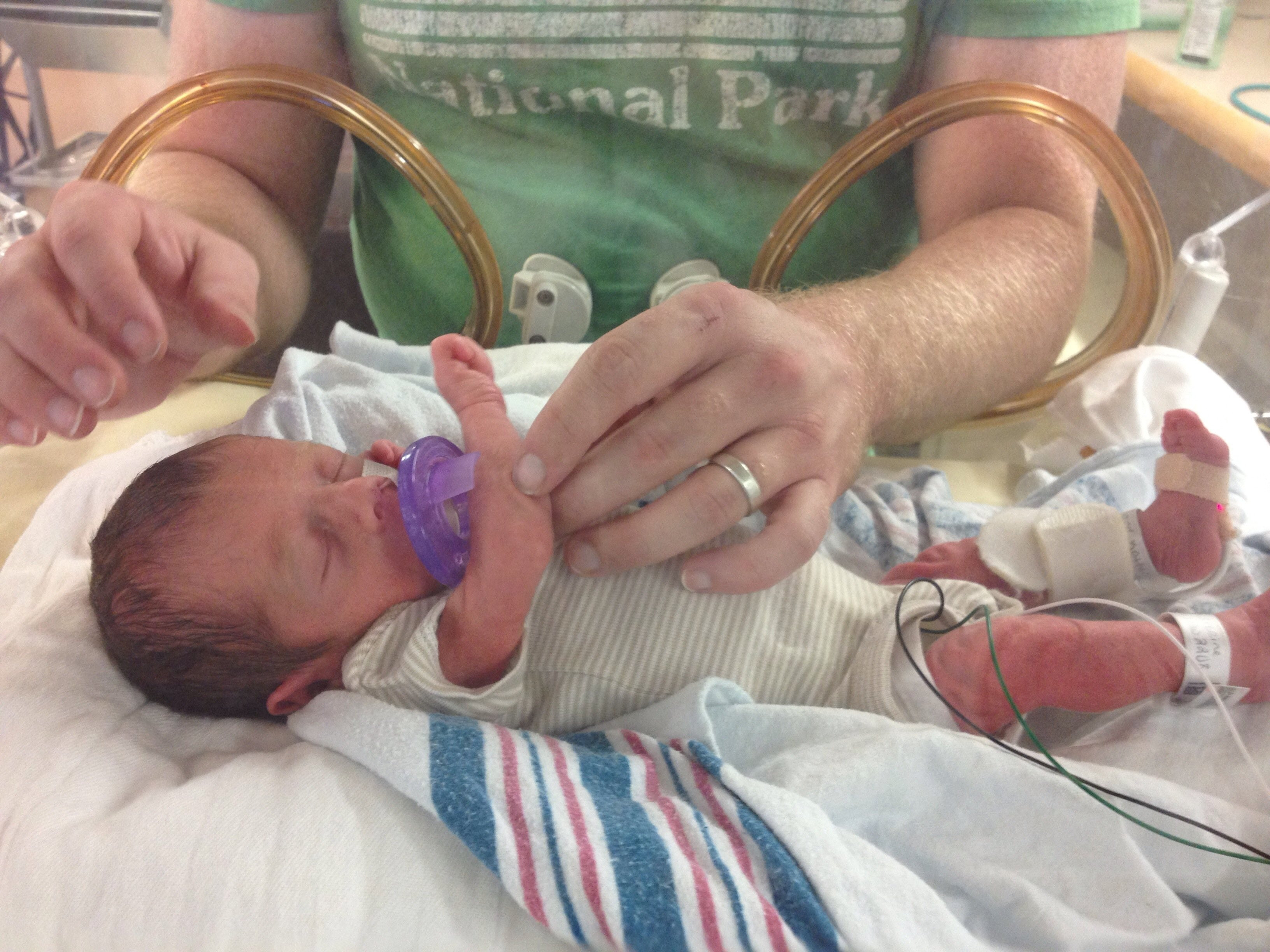
A few hours later, our son was born. He weighed just 2 pounds, 14 ounces.
But he was okay.
I couldn’t help but think about what might have happened—if I hadn’t gone to my prenatal appointments because I couldn’t afford to or couldn’t leave work.
Across the country, many parents can’t afford the pre-and postnatal care that saved our lives. In fact, women in the United States are more likely to die from complications related to pregnancy and childbirth than in any other industrialized nation. For Black women, the risk of pregnancy-related deaths is 3-4 times higher. For Indigenous women, 2-3 times higher.
And 15% of American women don’t receive adequate prenatal care. Their babies are three times more likely to have a low birth weight and five times more likely to die than those born to mothers who do get care.
The problem is that maternal health care is inequitable. For most, whether you and your child live or die during the birthing process is not about need, or about your right to good health, but about who you are, where you come from and how much money you make.
The systems that feed these disparities are complex, with roots that go back to our country’s founding. Fortunately, organizations like the National Birth Equity Collaborative (NBEC) are on the frontlines of improving care and raising awareness about the needs of all birthing people—whether it be advocating for a federal Office of Reproductive Wellbeing or removing restrictions on abortion like the “global gag rule.” NBEC is helping ensure the sexual reproductive health and well-being of Black women and birthing people worldwide.
Other organizations like the Illinois Perinatal Quality Collaborative work with hospitals, perinatal clinics, patients, public health leaders and policymakers to improve health care for mothers and babies. The Collaborative will soon launch an obstetric quality improvement initiative to engage hospitals in implementing strategies to address maternal health disparities and promote birth equity.
Today, our son is a healthy, happy, hilarious 8-year-old. That he was born so early barely registers with him.
I’m still somewhat at risk—particularly if we decided to have another baby. Fortunately, if we did, we’d be supported. By our family, doctors, jobs, and health care plan. We were lucky, but many aren’t, and I will never take that for granted.
A variation on this piece originally appeared on Scary Mommy. Read the full piece here.